Dermatological emergencies- Toxic epidermal necrolysis (T.E.N.)
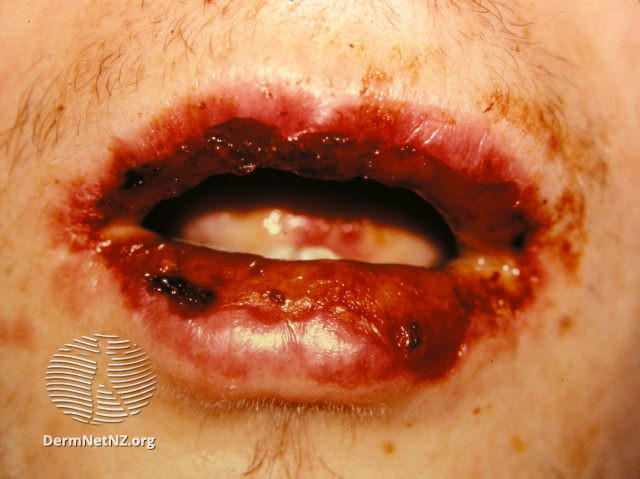
Toxic epidermal necrolysis (T.E.N.) has distinct clinical features, such as erythema that affects more than 30% of skin’s surface supported by mucosal involvement and fever (>38 °C). Erythema is followed by an extensive full-thickness mucosal and cutaneous necrosis (death of cells or tissues) and denudation that lasts 2-3 days. The similar symptoms and signs that involve less than 10% of the body surface are referred to Stevens-Johnson syndrome (SJS). If 10-30% of the body surface area affected by the symptoms mentioned above, it is referred to as T.E.N./SJS overlap.
The prodromal rash can be non-specific or can target certain lesions. It is followed by appearance of blisters filled with fluid that tend to spread with lateral pressure (Nikolsky’s sign) and eventually peel off which tends to reveal bright red oozing dermis. Shedding of hair and nails can occur as well.
The mechanism of T.E.N. is related to cell-mediated cytotoxic reaction caused against epidermal and activated by lymphocytes and their cytokines.
T.E.N. is a serious medical emergency that has a high mortality rate. It should be treated in intensive care facility or burn unit. However, by nature, it is quite a rare condition that has one per million incidence every year.
The acute graft versus host disease can also trigger occurrence of T.E.N. and effects are usually lethal.
The most common drugs that can cause T.E.N. are nonsteroidal anti-inflammatories, sulphonamides, allopurinol, and anticonvulsants (e.g. lamotrigine, carbamazepine, phenytoin).
The further investigations of T.E.N. are performed to study various complications associated with disease and explore the underlying causes. Skin swabs are done to detect presence of secondary bacterial infection. Other forms of investigation include full haematological and biochemical screen.
T.E.N. has a lot of complications on one’s health. This includes protein loss, difficulties with thermoregulation, dehydration, interstitial pneumonitis, neutropoenia, liver failure, heart failure, renal tubular necrosis , and eroded gastrointestinal tract.
SCROTEN is a specially designed illness severity score that helps physicians to predict mortality rate associated with T.E.N. and SJS cases. The criteria includes the following factors: age should be greater than 40 years old, malignancy should be present, heart rate above 120, initial epidermal detachment greater than 10%, serum glucose level greater than 14 mmol/L, serum urea level greater than 10 mmol/L, and serum bicarbonate level less than 20 mmol/L. Each criteria equals to one point. SCRTOTEN 0-1 means more than 3.2% of predicted mortality. SCRTOTEN 0-1 means more than 3.2% of predicted mortality. SCRTOTEN 2 means more than 12.1% of predicted mortality. SCRTOTEN 3 means more than 35.3% of predicted mortality. SCRTOTEN 4 means more than 58.3% of predicted mortality. Lastly, SCRTOTEN 5-7 means more than 90% of predicted mortality.
With presence of T.E.N. it is highly advised to discontinue taking any recently prescribed medications. Moreover, they should never be re-administrated in the future. The recurrent T.E.N. is much more severe that the initial outburst of T.E.N.
As previously mentioned, the management of T.E.N. is usually done in the intensive care unit where expert supportive care is available. The environment should be kept warm, fluid should be regularly replaced, and any electrolyte disturbances should be immediately corrected. Prevention of sepsis is done by introducing intravenous antibiotics. Other regulations include introduction of analgesics, mucosal emollients, and non-stick occlusive burns dressings.
The systemic corticosteroids should be avoided at all times because they increase the mortality rate. However, their usage still remains controversial.
The recovery process usually takes from 10 days to 3 weeks. The possible side effects include mucosal scarring and irregular pigmentation. Eye complications can also arise.
Due to COVID-19 eruption, Centre for Medical and Surgical Dermatology offers Teledermatology appointments from Mondays to Fridays.
For more information on Teledermatology, visit the following link: